Though protected by the eyelid and regularly lubricated each time we blink, the cornea is most likely to suffer injury or the “abuse of use.” Even the routine use of contact lenses can lead to keratitis—a painful inflammatory condition that can cause a reduction in the clarity of vision. In fact, contact lens wearers are often unaware of the serious complications and damage that can result from contact lens wear, damage that increases over time with continued use.
Chronic eye issues lead to corneal trauma, as well. Chronic infection, corneal erosion, and scarring can result in a corneal transplant.
One of the most common corneal pathologies is keratoconus. This condition is more prevalent in teenagers and young adults. Characterized by the thinning at its center, the cornea bulges outward, taking on a cone shape. Initially, the bulging changes how the cornea refracts light, resulting in refractive errors like astigmatism and nearsightedness. This condition can also cause inflammation, swelling, and (ultimately) scarring of the cornea. It usually affects both eyes,
All of the above can, of course, lead to varying degrees of impaired vision. Initially, eyeglasses can correct problems resulting from keratoconus, but as conditions worsen, patients may need custom contact lenses. Unfortunately, these can also contribute to damage in the long term.
Recently, corneal repair has gained popularity as a novel and effective vision correction solution. Currently available only from select physicians in the U.S., it has the potential to not only prevent your eyes from getting worse, but also to repair damage and correct your vision fully. No surgical procedure should be taken lightly. Still, anyone with issues involving their corneas should be mindful that the conditions they’re experiencing may well get worse over time.
While laser ablation is a very complex procedure, all the work is on the part of the laser surgeon and sophisticated technology. Not only must the surgeon be sufficiently skilled and experienced, but the precision laser and blade technology must be current. The surgeon goes through exacting steps to take the most precise measurement of the eye using this cutting edge technology.
Topographic guided ablation for corneal repair is a novel procedure that the US recently approved. It reconstructs the cornea by selectively removing the tissue that causes deformity in the cornea (warping). Whether the damaged cornea is due to trauma, corneal disease, or a poor surgical outcome (such as de-centered LASIK, PRK, or the distortion from radial keratotomy), the cornea can be re-normalized with Topographic Guided Ablation.
Pioneered by Dr. Manoj Motwani, the San Diego Protocol for topographic guided ablation is unique because it also incorporates knowledge gained in the LYRA Protocol. LYRA uses the same Contoura system used to create uniform corneas in primary laser vision correction to get rid of glasses and contacts, and can result in better than normal human vision.

Post-laser keratomileusis (LASIK) corneal ectasia is one of the most serious side effects of refractive surgery. It is characterized by a progressive thinning and steepening of the central and inferior portions of the cornea. Until recently, treatment options were limited to three main processes. These were using rigid contact lenses, inserting intrastromal rings to help mechanically stabilize the cornea, or undergoing penetrating keratoplasty.
Initially, physicians learned that the optimal solution for corneal ectasia was to correct the patient’s vision (rather than the underlying pathology) because they couldn’t do anything else. As a result, patients would see their disease progress until only a corneal transplant would solve it. That procedure poses higher risks.
Corneal cross-linking is a method of corneal repair that halts the eye’s progression from keratoconus. It makes a cornea transplant unnecessary. Instead of incrementally correcting vision and waiting until a transplant is needed, doctors can now strengthen the cornea and preserve its shape. While the procedure may not eliminate the need for contact lenses, it arrests cornea damage symptoms and the progression of corneal disease.
Unlike previous treatment options, corneal cross-linking (CXL) halts the progression of ectasia by improving the structural integrity of the cornea. Utilizing ultraviolet-A (UVA) light and a topical photosensitizer, the procedure creates new cross-links between collagen lamellae, strengthening the integrity of the cornea itself.
Candidates for corneal cross-linking should be diagnosed with keratoconus or irregular astigmatism. Their corneas must be at least 400 microns thick. Recovery from the procedure typically requires around one week. The patient will initially experience limited vision due to the healing process.
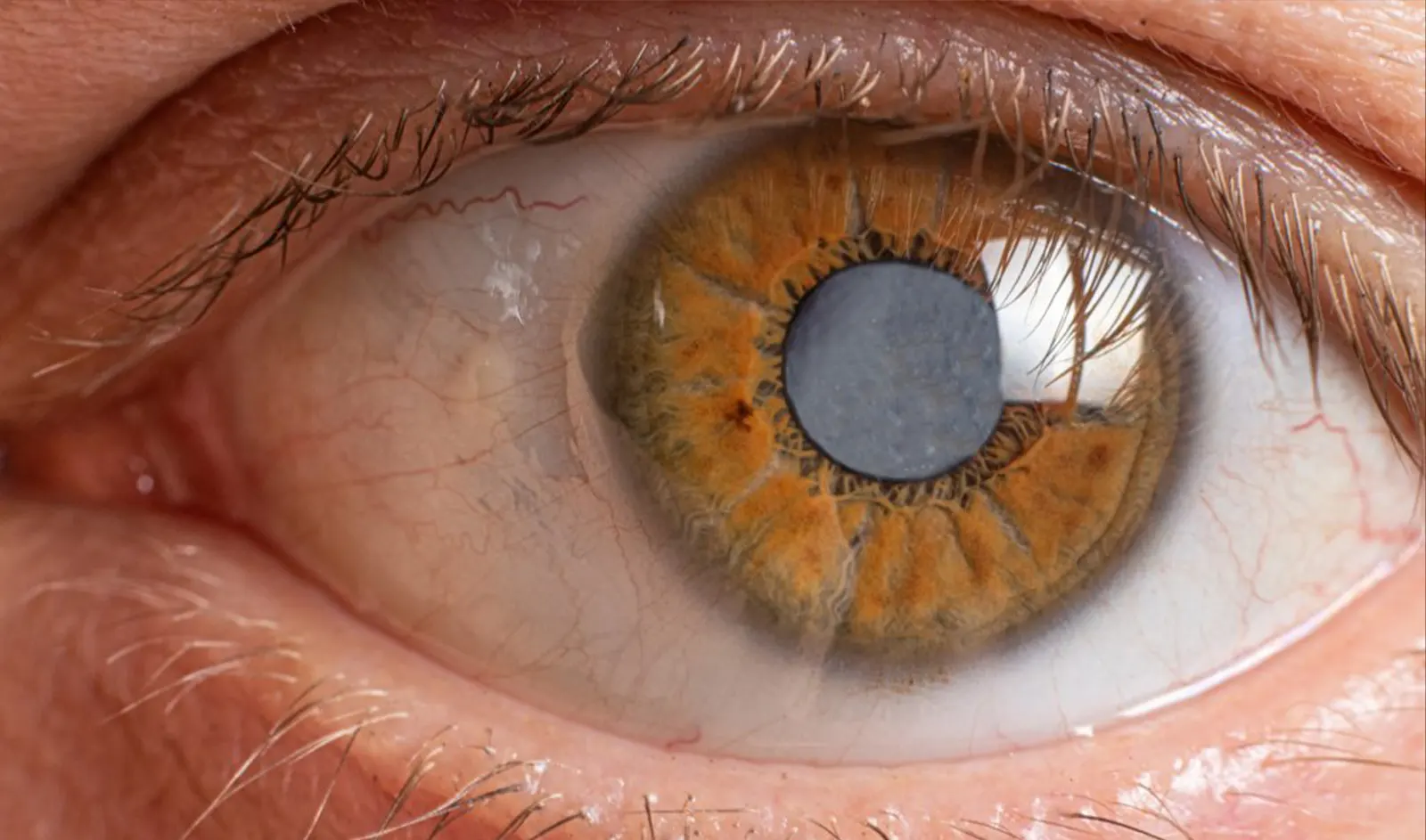
Cataract Surgery is the most performed surgical procedure in the United States, and has a phenomenal track record for improving…
Read More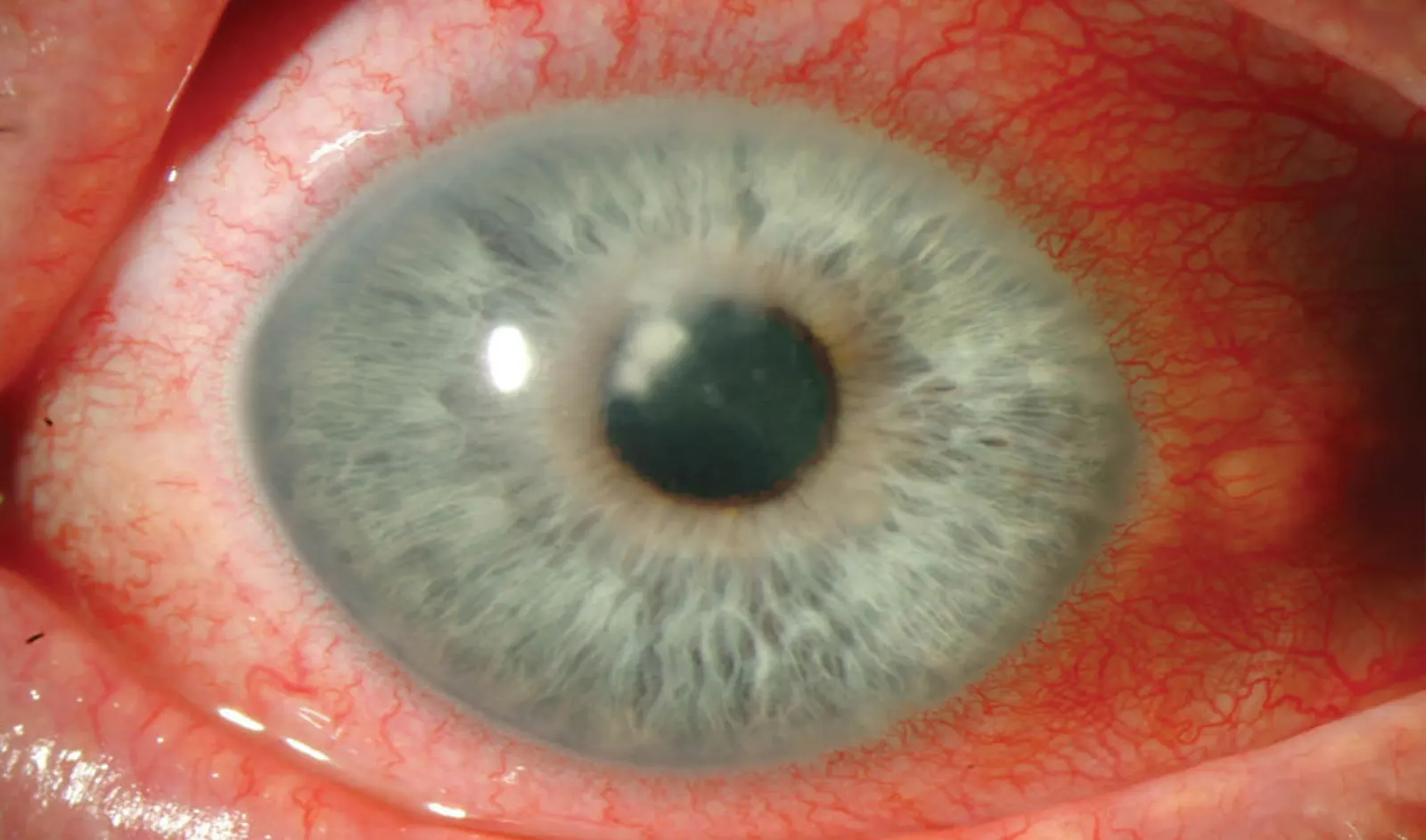
The treatment of trauma with topographic-guided ablation depends on the level of scarring caused by the trauma, the position of…
Read More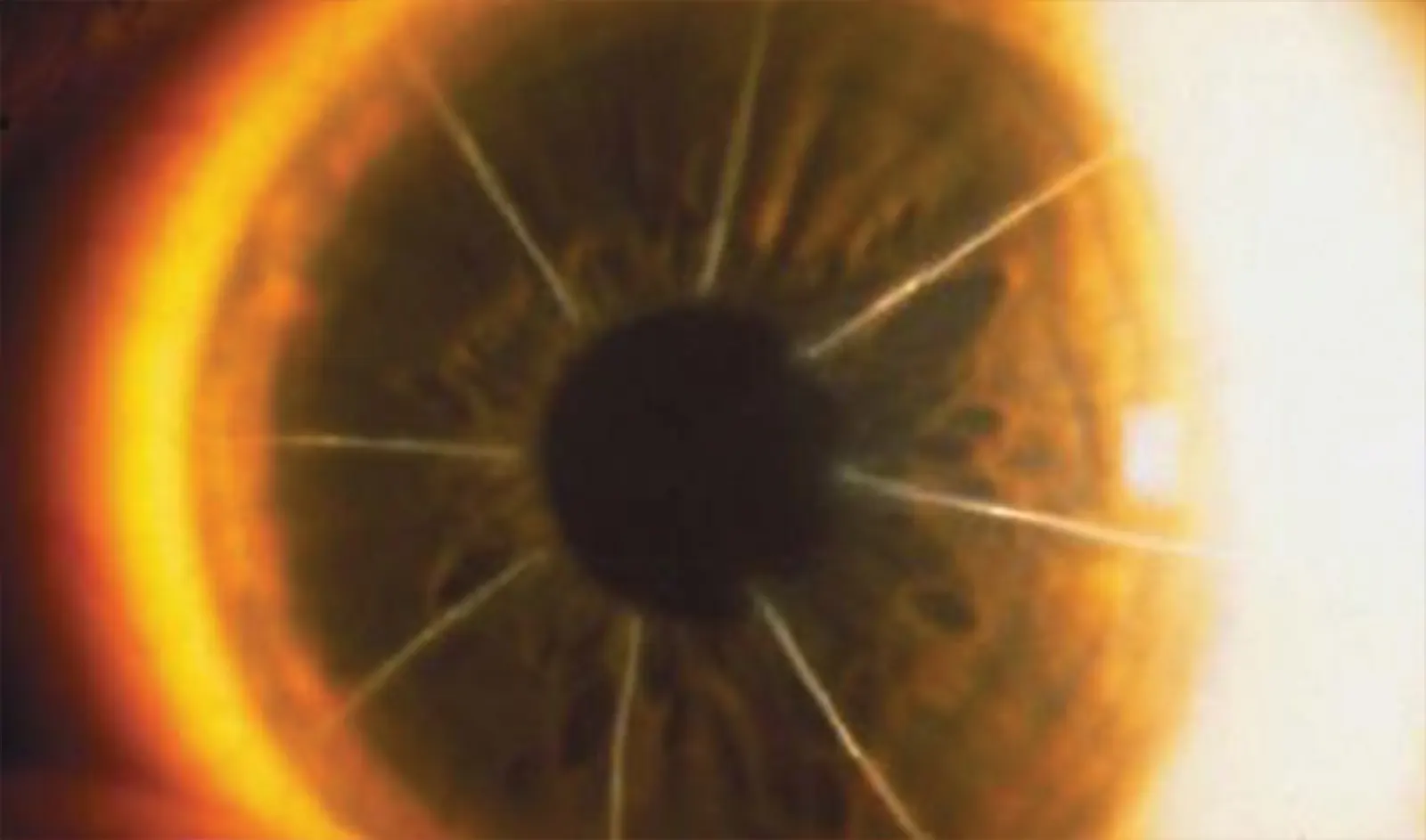
In the dynamic world of eye care, keratoconus treatment has become a focal point due to the condition’s impact on…
Read More