The cornea is the clear tissue on the front of the eye. It plays a protective role, shielding the eye from the environment. It also serves as the window of the eye, enabling clear vision when it is functioning optimally and efficiently. Unfortunately, that is not always the case. In certain advanced corneal conditions, a transplant may be required.
A corneal transplant involves grafting corneal tissue from a donor. In a full-thickness transplant, the patient’s central cornea is removed with the use of a circular cutting device called a trephine. The donor cornea is also trephined and inserted in the place of the removed tissue.
There are certain corneal conditions for which a transplant may be needed, such as keratoconus, bullous keratopathy, scars, ulcers, dystrophies, and post-LASIK ectasia. The goal of surgery is to replace the patient’s diseased or damaged cornea with healthy donor tissue, improving the clarity of vision.
Risks of corneal transplantation include rejection, infection, bleeding, glaucoma, and retinal detachment. Astigmatism is also a common corneal transplant complication.
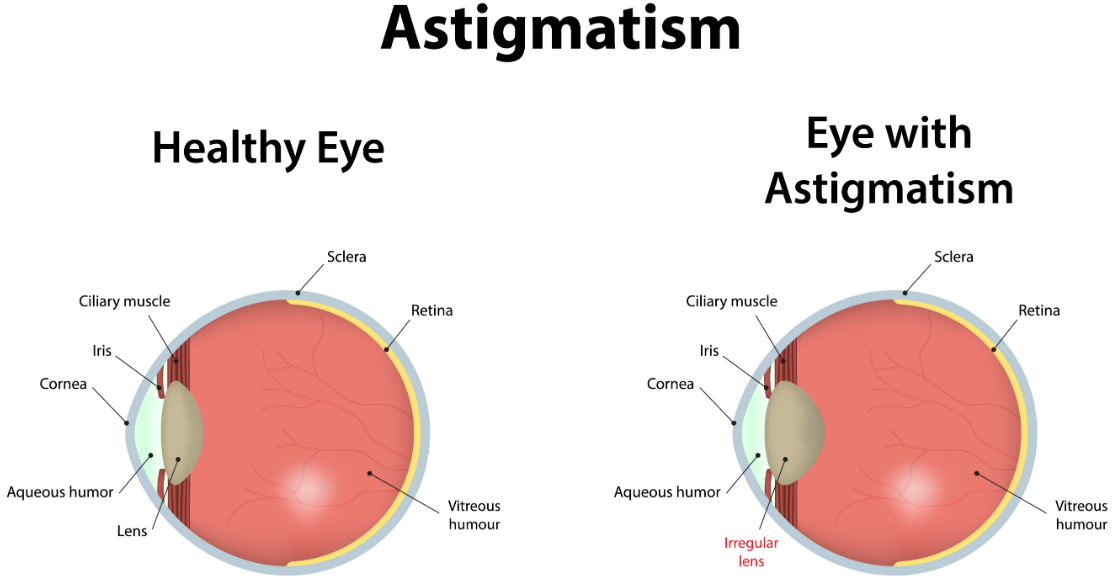
Astigmatism is a type of refractive error that can come from the cornea. Corneal astigmatism results when the curvature of the cornea in one direction is different than the curvature in another direction. Rather than the cornea being shaped like a perfectly round soccer ball, it resembles a football. This may result in blurry vision, headaches, eye strain, squinting, and difficulties with night vision.
Patients may end up with significant astigmatism after a corneal transplant. There are two types of astigmatism: regular and irregular.
Regular astigmatism is geometrically symmetrical and can usually be corrected with glasses or soft contact lenses. However, sometimes the amount of astigmatism after a transplant is so high that it makes this impractical.
Irregular astigmatism poses a significantly greater challenge because it is so detrimental to the vision and can’t be corrected in glasses or soft contact lenses. Irregular astigmatism can cause blur, halos, glare, and distortion. It can occur due to the fact that the grafted cornea is not the same shape or curvature as the original cornea, and because the grafted cornea needs to be sewn in by hand and the stitches can be uneven in tension. In those who have had a corneal transplant for keratoconus, irregular astigmatism may develop years after the initial surgery. This is because, without further intervention, their condition can continue to progress despite corneal transplantation. Gas-permeable contact lenses or certain surgical procedures can be used to correct irregular astigmatism. While gas-permeable contact lenses may be an option for some people, they are often not well tolerated. Furthermore, in order to truly correct the irregularity, surgical intervention is needed.
Astigmatism, whether regular or irregular, can be improved using laser corneal reconstruction. During this procedure, the ablation of corneal tissue is guided by topography, which provides a map of the curvature of the cornea, and selectively removes tissue to create a smoother, more uniform surface. This is especially useful for irregular astigmatism, as that is very difficult to treat.
The Wavelight Contoura system is the most powerful corneal topographic system available in the United States. Its approval by the Food & Drug Administration (FDA) includes use in corneal repair and treatment of irregularity and warpage. This means surgeons can now repair post-corneal transplant astigmatism through laser resurfacing.
Only the best corneal transplant surgeons in the United States have the technology and skill to achieve this. The goal in laser corneal reconstruction is to smooth out the surface of the cornea by removing the irregularities causing visual problems. With the aid of the Wavelight Contoura, each of the 22,000 discrete points on the cornea can be fine-tuned to the appropriate curvature. This allows for treatment to be truly customized to the individual.
In order to maintain results from laser corneal reconstruction, corneal cross-linking can be used as an adjunct procedure. This is especially important in keratoconus patients, who are at risk for progression of their disease after corneal transplantation. In all patients, corneal cross-linking helps to “freeze” the results, so vision remains stable for years after treatment. It uses ultraviolet light in combination with a photosensitizer, riboflavin, to cure the cornea. This improves the structural integrity of the cornea by strengthening the bonds between each layer of collagen. By improving the rigidity of the cornea, it is less prone to changing shape over time.
In order to be a candidate for cross-linking, patients must have a minimum corneal thickness of 400 microns. This will be measured by the clinic when assessing for candidacy. Patients should also expect their vision to be blurry for roughly a week following corneal cross-linking, as the tissue heals from the procedure.
Using laser corneal reconstruction combined with corneal cross-linking is the most advanced keratoconus treatment available, and is designed to prevent progression and the need for a corneal transplant.
When you’re not seeing properly through your corneal transplant, you may experience headaches, loss of reading ability, loss of ability to pursue interests, trouble driving, loss of independence, risk of injury, loss of employment prospects, and depression and anxiety. These are all reasons not to delay your corneal repair.
Dr. Motwani has removed irregular astigmatism with laser corneal reconstruction that helps decrease blurring, multiple images, and night vision issues to allow patients to see well, function well, work, and drive again. What are you waiting for? Book your consultation today.
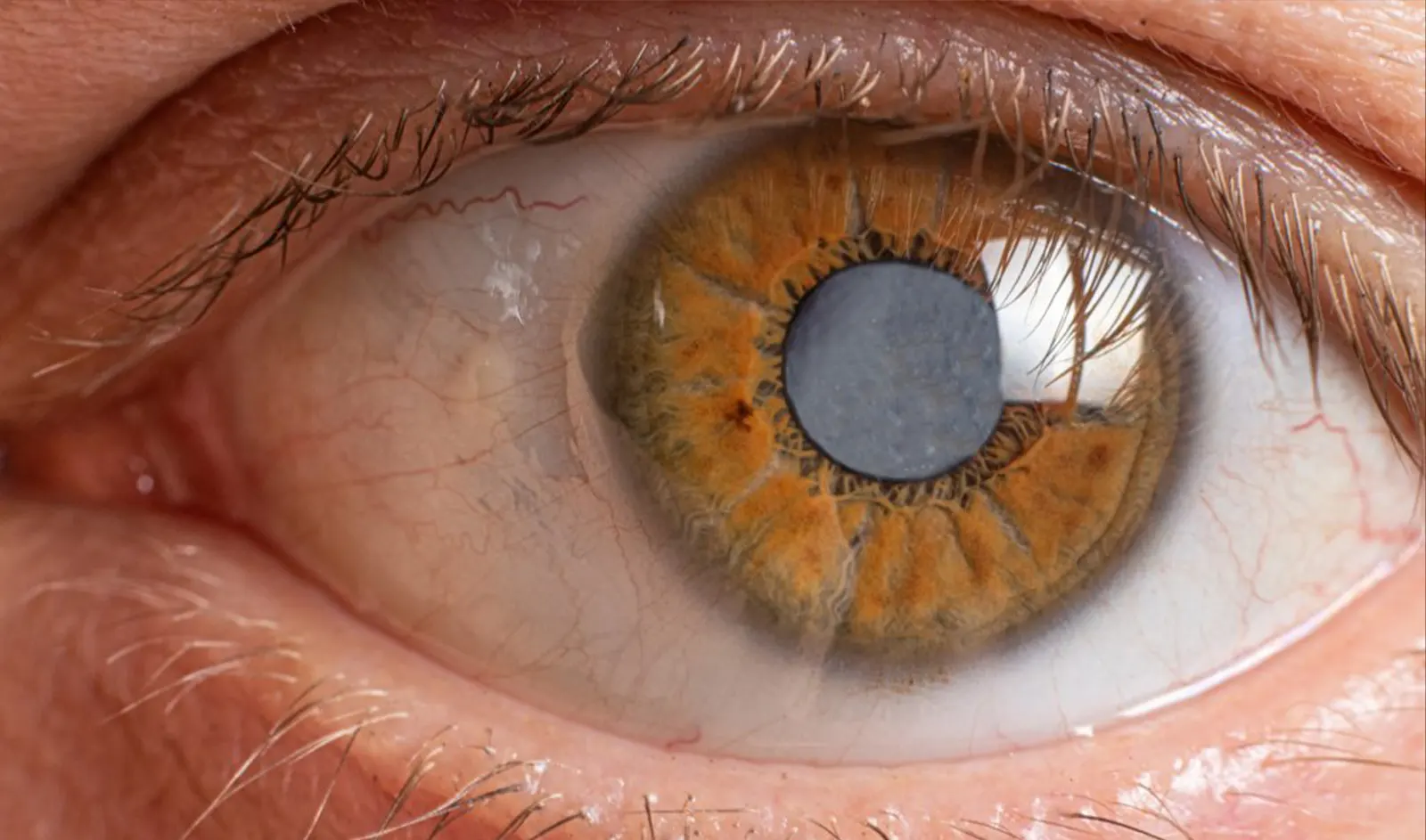
Cataract Surgery is the most performed surgical procedure in the United States, and has a phenomenal track record for improving…
Read More
The treatment of trauma with topographic-guided ablation depends on the level of scarring caused by the trauma, the position of…
Read More
In the dynamic world of eye care, keratoconus treatment has become a focal point due to the condition’s impact on…
Read More